Westminster Politics 2024-2029
- Thread starter Pexbo
- Start date
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Frosty
Logical and sensible but turns women gay
Good. Get it done. We seemingly are incapable of wholesale reform of the Lords, so it does make sense to carry things out piecemeal and focus on the things which no one can politically reverse.
At this stage in the election cycle, that is totally meaningless.
Nogbadthebad
Full Member
Bastani also posted a piece I hadn;t noticed about where this much vaunted investment is coming from.
Fresh from their success in milking thames water for around a half a billion and leaving the state to pick up the tab, Maquarie are back for some more of your money.
Fresh from their success in milking thames water for around a half a billion and leaving the state to pick up the tab, Maquarie are back for some more of your money.
Nogbadthebad
Full Member
At this stage in the election cycle, that is totally meaningless.
12 weeks ago, starmer was still much of a mystery to the public, little coverage of his dishonesty or murky relationships with very rich people.
Now they see him, because it can't be hidden and they don't like it.
Guaranteed that he will face a leadership challange before the next election with these numbers, I'd guess 2028 to give the new one time to bed in before an election. Reeves or Streeting is most likely, but if mcsweeney puts himself up for election in a by election in 2026-27, put money on it being him.
Sweet Square
ˈkämyənəst
This is private investment into the Labour Party, a fraction will reach public projects.
FireballXL5
Full Member
- Joined
- May 9, 2015
- Messages
- 10,880
Plus ça change.
Maticmaker
Full Member
- Joined
- Nov 8, 2018
- Messages
- 5,326
He's continuing to 'pick his battles', which is a good sign.Good. Get it done. We seemingly are incapable of wholesale reform of the Lords, so it does make sense to carry things out piecemeal and focus on the things which no one can politically reverse.
The winter fuel payments was a 'left-hook to the left' and the VAT on Private Schools was a 'right-hook to the right' and it was a 'straight-left to the jaw' of both Louise Haigh and Angela Rayner over the PO damage limitation issue, and a warning to other cabinet members, to think before they speak, especially when being interviewed live.
This man is serious.
Exactly. As long as he keeps a look out for 'leg-traps' set by his own party especially those who tend to mumble in their beer/make bullets for others to fire.At this stage in the election cycle, that is totally meaningless.
This man is not afraid to take fire from both sides.... sometimes even at one and the same time.
Sweet Square
ˈkämyənəst
Dancfc
Full Member
- Joined
- Oct 28, 2016
- Messages
- 7,639
- Supports
- Chelsea
Three months is all it's took for this public to forget about the last 14 years.
We deserve everything we get at this point.
Smores
Full Member
- Joined
- May 18, 2011
- Messages
- 26,584
He's continuing to 'pick his battles', which is a good sign.
The winter fuel payments was a 'left-hook to the left' and the VAT on Private Schools was a 'right-hook to the right' and it was a 'straight-left to the jaw' of both Louise Haigh and Angela Rayner over the PO damage limitation issue, and a warning to other cabinet members, to think before they speak, especially when being interviewed live.
This man is serious.
Exactly. As long as he keeps a look out for 'leg-traps' set by his own party especially those who tend to mumble in their beer/make bullets for others to fire.
This man is not afraid to take fire from both sides.... sometimes even at one and the same time.
Winter fuel payment a left hook to the left


Berbasbullet
Too Boring For A Funny Tagline
- Joined
- Nov 3, 2011
- Messages
- 22,825
I’m not sure taking fire from both sides is a good thing though is it?He's continuing to 'pick his battles', which is a good sign.
The winter fuel payments was a 'left-hook to the left' and the VAT on Private Schools was a 'right-hook to the right' and it was a 'straight-left to the jaw' of both Louise Haigh and Angela Rayner over the PO damage limitation issue, and a warning to other cabinet members, to think before they speak, especially when being interviewed live.
This man is serious.
Exactly. As long as he keeps a look out for 'leg-traps' set by his own party especially those who tend to mumble in their beer/make bullets for others to fire.
This man is not afraid to take fire from both sides.... sometimes even at one and the same time.
How is winter fuel payments an attack on the left?
I suppose these Twitter accounts have to post something like this; its their raison d'être. But never mind what poll might imply, who are the respondents that are providing a valid response this far out from an election? It seems as hypothetical as preferences for a govt can get, somewhat akin to a poll in a country where people may never get to vote at all.
- Joined
- Oct 22, 2010
- Messages
- 23,904
I suppose these Twitter accounts have to post something like this; its their raison d'être. But never mind what poll might imply, who are the respondents that are providing a valid response this far out from an election? It seems as hypothetical as preferences for a govt can get, somewhat akin to a poll in a country where people may never get to vote at all.
are you unfamiliar wth opinion polling?
polling for 2024 started in jan 2020
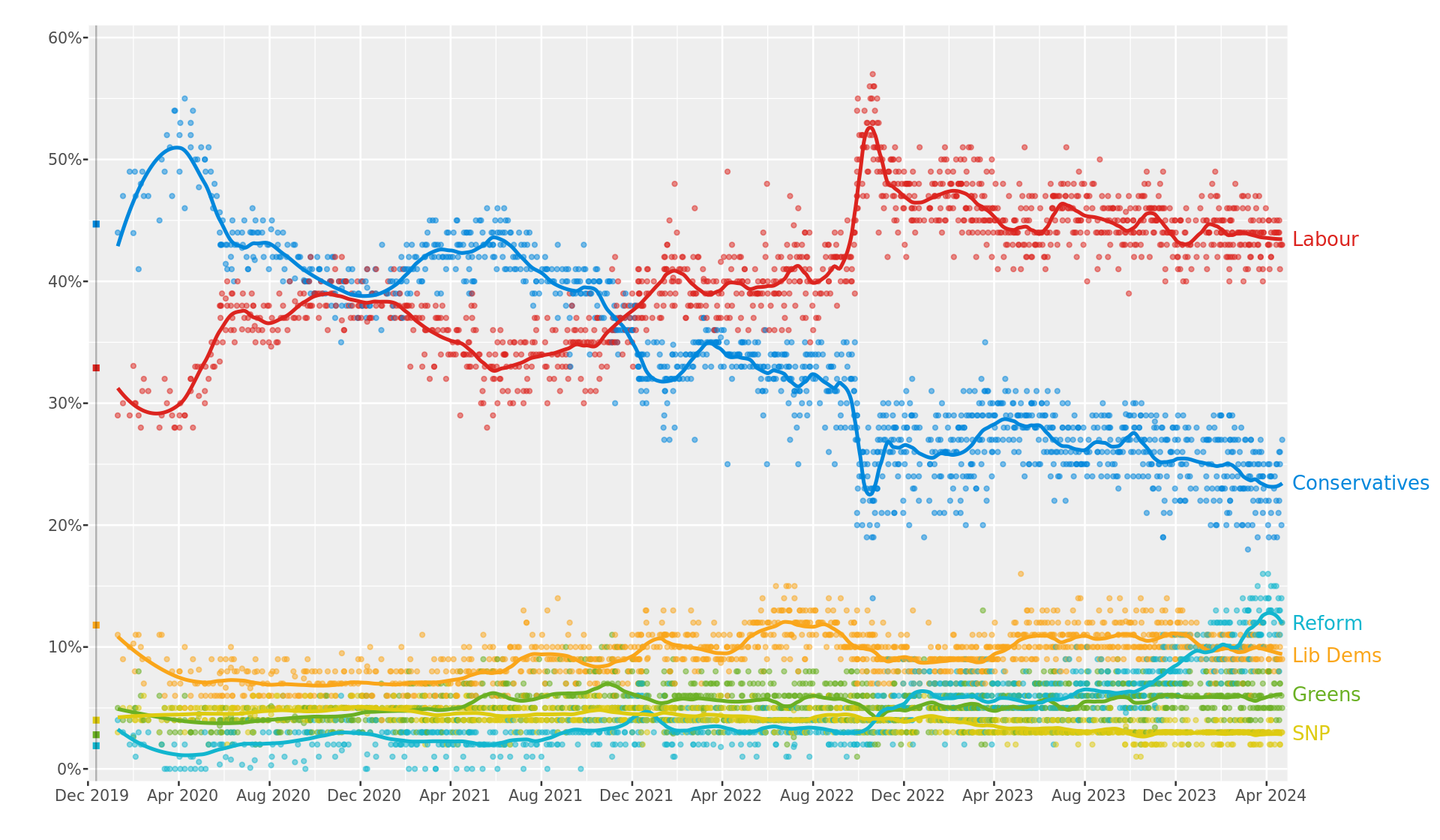
No need to be patronising: You just could try addressing my question. Anyhow, maybe your graph does show the irrelevance of polls this far out from the actual election.are you unfamiliar wth opinion polling?
polling for 2024 started in jan 2020

- Joined
- Oct 22, 2010
- Messages
- 23,904
No need to be patronising: You just could try addressing my question. Anyhow, maybe your graph does show the irrelevance of polls this far out from the actual election.
they're irrelevant about 2029 but are very relevant in judging the mood of the public towards the govt. and newly sworn in government typically get a bump, while the starmer govt has got the opposite.
No new manager bounce then. The country's very own Erik Ten Bags (of free stuff)they're irrelevant about 2029 but are very relevant in judging the mood of the public towards the govt. and newly sworn in government typically get a bump, while the starmer govt has got the opposite.
- Joined
- Oct 22, 2010
- Messages
- 23,904
No new manager bounce then. The country's very own Erik Ten Bags (of free stuff)
i think theresa may had stangant/bad polling after the 2017 election, but from the uk i dont remember a drop anything like this.
(basically the best comparison may be ralf rangnick
 )
)nickm
Full Member
- Joined
- May 20, 2001
- Messages
- 9,800
Sure, man. Like you can draw any conclusions about a 5 year term 100 days in.12 weeks ago, starmer was still much of a mystery to the public, little coverage of his dishonesty or murky relationships with very rich people.
Now they see him, because it can't be hidden and they don't like it.
Guaranteed that he will face a leadership challange before the next election with these numbers, I'd guess 2028 to give the new one time to bed in before an election. Reeves or Streeting is most likely, but if mcsweeney puts himself up for election in a by election in 2026-27, put money on it being him.
FireballXL5
Full Member
- Joined
- May 9, 2015
- Messages
- 10,880
Cutting red tape...now where have we heard that one before?
Unions express concern as PM to say government will ‘rip out the bureaucracy that blocks investment’
https://www.theguardian.com/politic...rmer-promise-slash-red-tape-investment-summit
Keir Starmer will promise to slash red tape as he hosts investment summit
Unions express concern as PM to say government will ‘rip out the bureaucracy that blocks investment’
https://www.theguardian.com/politic...rmer-promise-slash-red-tape-investment-summit
Dobba
Full Member
The final Grenfell inquiry report isn't even six weeks old and Starmer is fantasising about cutting red tape around building.
TheGame
Full Member
This is not normal.
TheGame
Full Member
Guarantee they will will have given tours to some seriously nefarious characters. Russian and Israelis no doubt that just wanted a bit of sightseeing.
Frosty
Logical and sensible but turns women gay
At the Conservative conference Badenoch’s team released a 36-page essay called Conservatism in Crisis which identifies many factors supposedly holding back growth. On anxiety and autism it says:
It is a positive thing our society is now more open around mental health. However, the socialisation of mental health, whereby mental health moved from something that people worked on for their own benefit, to something where everyone had to treat you differently, has both created costs and failed to improve people’s mental health outcomes ….
[A change in the perception of harm] helps explains why people who had suffered events once seen as non-traumatic now feel entitled to support. This increases demand for psychologists and therapists, required to help people previously seen as able to cope. As will be set out in the forthcoming book [based on the essay] across the psychological and psychotherapy professions, numbers have risen from 102,000 in 2002 to 223,700 in 2023.
Being diagnosed as neuro-diverse was once seen as helpful as it meant you could understand your own brain, and so help you to deal with the world. It was an individual focused change. But now it also offers economic advantages and protections. If you have a neurodiversity diagnosis (e.g. anxiety, autism), then that is usually seen as a disability, a category similar to race or biological sex in terms of discrimination law and general attitudes.
If you are a child, you may well get better treatment or equipment at school – even transport to and from home. If you are in the workforce, you are protected in employment terms from day 1, you can more easily claim for unfair dismissal, and under disability rules you can also require your employer makes ‘reasonable adjustments’ to your job (and you can reveal your disability once you have been employed rather than before).
In short, whereas once psychological and mental health was seen as something that people should work on themselves as individuals, mental health has become something that society, schools and employers have to adapt around.
Maticmaker
Full Member
- Joined
- Nov 8, 2018
- Messages
- 5,326
Yes, it is, because it means he is serious about what he is doing and is not going to be put off by sniping from either side.I’m not sure taking fire from both sides is a good thing though is it?
How is winter fuel payments an attack on the left?
Also at the moment having withdrawn the whip from some (suspect there will be others to come) who were taking 'pot shots' at him almost before he had got behind the PM desk in No.10, he is making full use of his position, i.e. that of a Labour PM with a massive majority.
Because it is a sign he is willing to take hard decisions, which will inflame many on the left; it could have been handled better but when you see what happened with Grey, it tends to explain how wires might have got crossed.
The VAT on Private schools was also a 'warning shot across the bows' of the right, signalling... "I am coming for you too", eventually!
All he needs to worry about is outside the UK; storms breaking in the Middle East, a new President in the USA, what is likely to happen in the Ukraine, anything external that can blow him of course. Internally, he can ride out almost anything.
Sweet Square
ˈkämyənəst

Berbasbullet
Too Boring For A Funny Tagline
- Joined
- Nov 3, 2011
- Messages
- 22,825
So I have it straight, removing the winter fuel allowance upsets the left because it demonstrates that Starmer is willing to make hard choices?Yes, it is, because it means he is serious about what he is doing and is not going to be put off by sniping from either side.
Also at the moment having withdrawn the whip from some (suspect there will be others to come) who were taking 'pot shots' at him almost before he had got behind the PM desk in No.10, he is making full use of his position, i.e. that of a Labour PM with a massive majority.
Because it is a sign he is willing to take hard decisions, which will inflame many on the left; it could have been handled better but when you see what happened with Grey, it tends to explain how wires might have got crossed.
The VAT on Private schools was also a 'warning shot across the bows' of the right, signalling... "I am coming for you too", eventually!
All he needs to worry about is outside the UK; storms breaking in the Middle East, a new President in the USA, what is likely to happen in the Ukraine, anything external that can blow him of course. Internally, he can ride out almost anything.
Frosty
Logical and sensible but turns women gay
USS is the universities pension scheme.
Good luck with asking university staff for money given the state of HE.
nickm
Full Member
- Joined
- May 20, 2001
- Messages
- 9,800
It should be possible to cut red tape around building infrastructure without turning every new appartment block into a potential bonfire.The final Grenfell inquiry report isn't even six weeks old and Starmer is fantasising about cutting red tape around building.
We don't build enough of anything in this country, quickly enough and we have to address it as a priority.
Maticmaker
Full Member
- Joined
- Nov 8, 2018
- Messages
- 5,326
Broadly speaking yes, there were many faults with a system that devotes millions to those who really don't need it, as well as those who do. It was a hard-nosed decision, which could have been handled differently, but it was important to Starmer to show he will take such decisions.So I have it straight, removing the winter fuel allowance upsets the left because it demonstrates that Starmer is willing to make hard choices?
All my personal acquaintances, who are very left of centre, are all 'spitting feathers', over this...which tends to confirm my suspicions there was some method in his apparent madness.
Dobba
Full Member
It should be possible to build a high-rise building, in one of the richest countries on the planet, without strapping kindling to the sides so it looked nicer for the neighbours. But here we are.It should be possible to cut red tape around building infrastructure without turning every new appartment block into a potential bonfire.
We don't build enough of anything in this country, quickly enough and we have to address it as a priority.
And apparently where we are is still too covered in red tape for Starmer's liking.
Berbasbullet
Too Boring For A Funny Tagline
- Joined
- Nov 3, 2011
- Messages
- 22,825
Interesting because I felt the outrage was more from the right.Broadly speaking yes, there were many faults with a system that devotes millions to those who really don't need it, as well as those who do. It was a hard-nosed decision, which could have been handled differently, but it was important to Starmer to show he will take such decisions.
All my personal acquaintances, who are very left of centre, are all 'spitting feathers', over this...which tends to confirm my suspicions there was some method in his apparent madness.
nickm
Full Member
- Joined
- May 20, 2001
- Messages
- 9,800
I agree, but I don't see what Grenfell has to do with abolishing a planning rule that makes it hard to build a data centre by the M25.It should be possible to build a high-rise building, in one of the richest countries on the planet, without strapping kindling to the sides so it looked nicer for the neighbours. But here we are.
And apparently where we are is still too covered in red tape for Starmer's liking.
Maticmaker
Full Member
- Joined
- Nov 8, 2018
- Messages
- 5,326
I agree it can be confusing. It seems that in advance of this much anticipated budget and constant references to this £22B 'black hole'. Starmer has chosen an odd mix of things to action, or not action, as the case maybe.Interesting because I felt the outrage was more from the right.
Refusal to move on the child allowance cap;
Announcing VAT to be levied on private schools;
Removal of Winter Allowance (except for those receiving Pension credit);
The proposed Non-Dom taxation system;
The decision to settle outstanding strikes in the public sector, above inflation
All the above, perhaps with the exception of the winter allowance, could be reasonably assumed to inflame elements specifically on the left, or the right.
Where as there is a perception that older folk would tend to be more right-leaning and therefore upset about the winter allowance, that has not been my personal experience. Those of my acquaintances (on the right) tend to think it is the right thing to do, but those who are very left wing, think it's disgraceful.... go figure!
Red in STL
Turnover not takeover
And what do pensions schemes do? They invest, it's not about more money, it's about where the money is invested for the benefit of both partiesUSS is the universities pension scheme.
Good luck with asking university staff for money given the state of HE.
Frosty
Logical and sensible but turns women gay
Mostly in Thames Water, sadly.And what do pensions schemes do? They invest, it's not about more money, it's about where the money is invested for the benefit of both parties
And both universities and university staff have a say in the management of the scheme. This will lead to industrial unrest if they are not careful.
I suspect you don't know many pensioners who have little private pension and are surviving on not much more than the pension credit threshold. These are the people that have been shat on. Yesterday one friend, a Labour voter, claimed Starmer had lost the next election already because of it. I understand the anger, she is genuinely struggling financially and this withdrawal will make a difference. I can only hope Labour realise they have made a mistake and set about correcting it, at least they have several years to do so.I agree it can be confusing. It seems that in advance of this much anticipated budget and constant references to this £22B 'black hole'. Starmer has chosen an odd mix of things to action, or not action, as the case maybe.
Refusal to move on the child allowance cap;
Announcing VAT to be levied on private schools;
Removal of Winter Allowance (except for those receiving Pension credit);
The proposed Non-Dom taxation system;
The decision to settle outstanding strikes in the public sector, above inflation
All the above, perhaps with the exception of the winter allowance, could be reasonably assumed to inflame elements specifically on the left, or the right.
Where as there is a perception that older folk would tend to be more right-leaning and therefore upset about the winter allowance, that has not been my personal experience. Those of my acquaintances (on the right) tend to think it is the right thing to do, but those who are very left wing, think it's disgraceful.... go figure!
Share:
